Cold, Flu, or COVID?
– Cough! Cough! Sneeze! –
“Stay away from me… You better get tested for COVID!”
“No, don’t worry. That sounds like a cold!”
“Are you sure it’s not bronchitis?”
“You know, it’s October – it could be the flu!”
Here we go again: Our annual battle with the sniffles that pops up in the Fall and continues into Winter. As if the cold vs. flu dilemma weren’t hard enough, now there’s COVID to wrap our heads around. We wanted to share some information on distinguishing one from another and some courses of action.
Before we dive into the good stuff, time for a quick anatomy lesson. You know how sometimes you get diagnosed with an upper respiratory infection? What exactly does that mean? And does that imply that there are lower respiratory infections, too? The answer is yes!
The respiratory tract itself is any part of the body that is responsible for the passage of air to and from the lungs. The upper respiratory tract includes our nose, sinuses, throat (pharynx), and our voice box (larynx). The lower respiratory tract starts at the trachea, extends through our bronchi, and ends in our lungs. That’s all there is to it. You are now officially an expert of the respiratory tract!
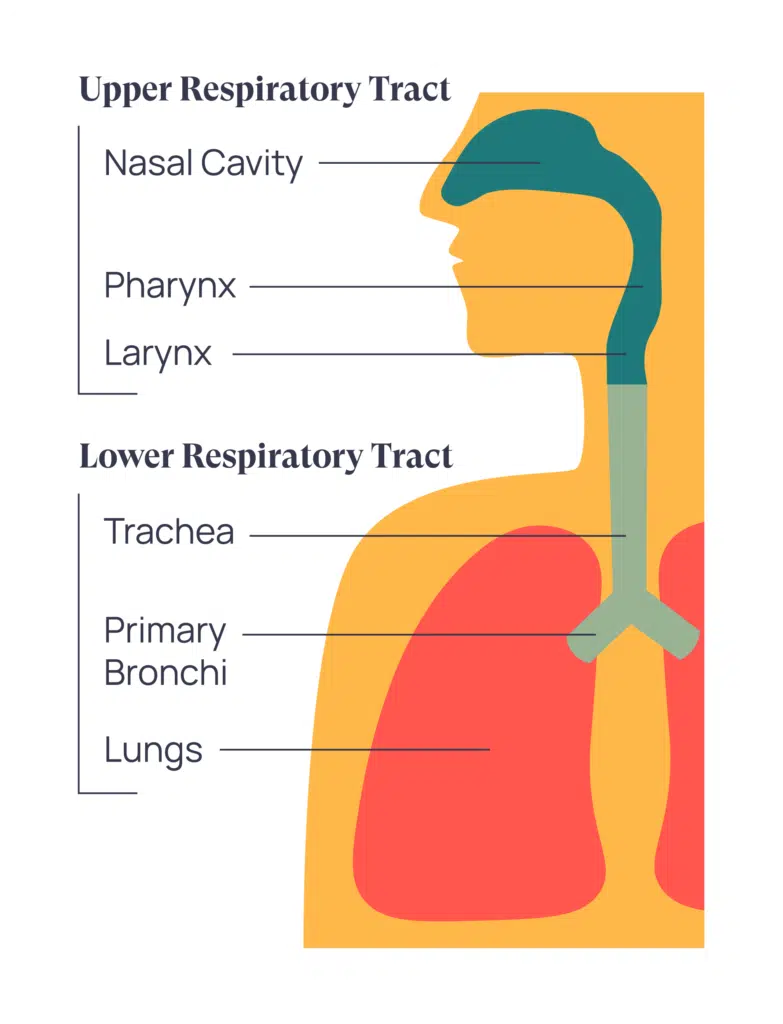
The common symptoms for upper respiratory infections (also called URI’s) are:
- Either no or low-grade fever
- Headache
- Nasal congestion
- Sneezing
- Sore throat
- +/- Loss of voice
URI’s are often caused by the common cold. There are actually several viruses that can cause the common cold such as Adenovirus, Rhinovirus, Coronavirus, and RSV. Another common cause of URI’s is the flu (also called Influenza).
“Back up real quick! Did you just say Coronavirus?!”
Yes! More on that in a little bit!
Lower respiratory tract infections tend to be more severe than URI’s. These infections are more commonly referred to by their anatomic location, the most common ones being bronchitis (when confined to the bronchi) and pneumonia (when the infection has travelled all the way down into the lungs). Common symptoms of these infections are:
- Moderate-to-high fevers
- Muscle aches
- Fatigue
- Coughing (oftentimes with phlegm)
- Shortness of breath
- Burning or sharp chest pain when coughing
Because the symptoms of both bronchitis and pneumonia are the same, they are differentiated by findings on either a lung examination or chest X-ray. Similar to URI’s, infections of the lower respiratory tract are also commonly caused by viruses.
“So what about bacteria and other germs?”
Yes, a very good question. You’ll see that most respiratory infections are caused by viruses. And the treatment is to attend to the symptoms while the body’s immune system dispels the virus. The usual mainstays of therapy are:
- Get plenty of rest
- Increase hydration
- Nasal saline irrigation
- Throat lozenges
- Ibuprofen or Tylenol for pain & fever control
You’ll notice that the list does not include antibiotics. Antibiotics are only effective against bacteria. Though bacteria can infect any part of the respiratory tract, their prevalence as the cause of infection is significantly lower than that of viruses. This is why your healthcare team is cautious about prescribing antibiotics when you become ill. They are unlikely to provide any benefit. More so, as bacteria have evolved through the years, their exposure to unnecessary antibiotics has actually made them harder to treat. In fact, the CDC reports that at least 2.8 million people each year get an antibiotic-resistant infection.
With all this said, if a bacteria is causing a respiratory infection, it is far more common to occur in the lower respiratory tract than the upper tract. And of lower respiratory tract infections, pneumonia is more likely to be caused by a bacteria than bronchitis. So frequently, your provider may opt to treat you with antibiotics if they believe you have pneumonia. For cases in which bronchitis lingers for three weeks, the medical literature recommends that antibiotics should then be used.
To recap so far, we’ve talked about the two parts of the respiratory tree, the differences in symptoms between the two types of infection, how to differentiate bronchitis from pneumonia, and when to use antibiotics. Now, let’s conclude with a discussion of cold vs. flu vs. COVID.
Let’s actually start with COVID (or COVID-19 as it is more properly known). COVID-19 is short for Coronavirus Disease – 2019. Coronavirus is a family of viruses that has been around for a very long time and, as mentioned earlier, is a prevalent cause of URI’s like the common cold. COVID-19 is a new type of Coronavirus, and most people who become infected with it experience symptoms of the common cold. But because it is stronger than other types of Coronavirus, sometimes it travels further down the respiratory tract and causes either bronchitis or pneumonia.
So based on symptoms, how can you tell when you have COVID? Unfortunately, you cannot. Because COVID can cause either an upper or lower respiratory tract infection, you need to obtain a test in order to determine if any type of respiratory symptom you may have is caused by COVID. (And PCR tests are the gold standard compared to antigen tests.)
So what about differentiating the cold vs. the flu? Well, this is tricky as well because both are causes of URI’s. As a result, there is a considerable overlap of symptoms. In thinking back to pre-COVID times, you might remember how often we would recommend flu testing when people had respiratory infections because it is difficult to diagnose purely by symptoms. But with that said, unlike the common cold, the flu has the ability to make its way into the lower respiratory tract. So by comparison, the flu causes more intense symptoms and is often characterized by:
- An abrupt onset more than a gradual onset
- Low-grade fever as opposed to no fever
- More intense headaches
- Muscle aches
- Chills
- Cough
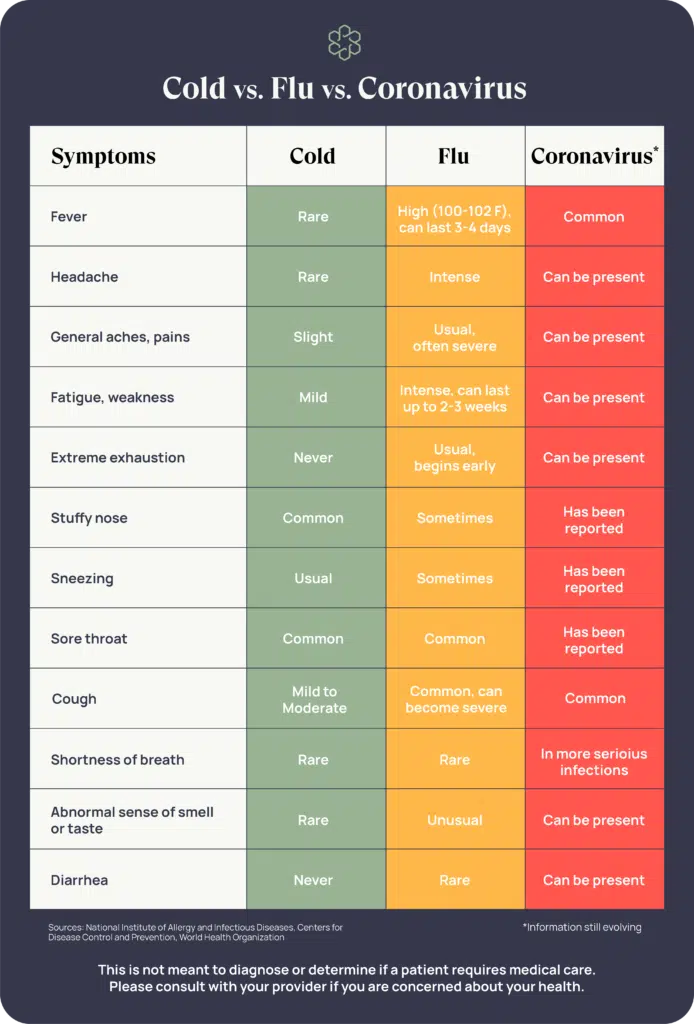
For a quick overview regarding the Cold vs. Flu vs. COVID, this table with information from UT Health Houston is very informative. Please note that this table is not intended for self-diagnosis!
And there you have it! If you have any questions or concerns, do not hesitate to reach out to a healthcare professional. Recognizing the differences between a cold, flu or COVID is tricky, and there is a lot of information to keep up with. If you haven’t been vaccinated against COVID yet or it’s time for your booster, go out and schedule an appointment today. And if you haven’t received your yearly flu shot, now is the perfect time to get one. We here at CareHive see all the great work you’re doing out there to stay safe – keep it up as the cool weather rolls in and flu season begins!
Suneet Singh, MD, FACEP // Medical Director, CareHive // Assistant Professor of Surgery & Perioperative Care, University of Texas at Austin Dell Medical School